Vestibular Assessment: Vertigo
The assessment of a patient complaining of dizziness, light headedness, vertigo, or unteadiness is often a daunting challenge. However, with a targeted history and systematic examination, the cause of the patients symptoms is almost always identified, a treatment program instituted or appropriate referral made. Difficult cases often require a multi-disciplinary approach to investigation and management.
Vertigo is the false sense of motion.. This is classically rotatory, but can manifest as translational movement. It is the result of an imbalance of activity in either the peripheral or central vestibular pathways.
Vertigo is often used interchangeably with dizziness. Dizziness, however, is a non-specific term used to encompass any imbalance in the integration of multiple inputs contributing to the orientation of the head and body in space. The main components of this system comprise the visual, vestibular and proprioceptive systems, with their central interconnecting processing centres. When these inputs disagree dizziness occurs
There is an extensive list of causes of dizziness most of which can be compartmentalised. Pre-syncopal dizziness [cardiogenic and orthostatic], ocular dizziness, drug induced dizziness, metabolic [most commonly hypoglycaemic], multisystem sensory dizziness, physiologic dizziness, anxiety related dizziness, dysequilibrium and vertigo, and an important classification termed psychophysiologic dizziness.
Importantly there is no mechanism through which abnormalities of the vestibular system can cause a loss of consciousness.
As a matter of definition peripheral vestibular system lesions arise from either within the labyrinth or the VIIIth cranial nerve. Central lesions occur either at the brainstem or higher levels.
The assessment and management of any patient suspected of suffering from vertigo, begins with a careful history. The patients own description of their symptoms is often invaluable.
Checklist on History
- Otologic: Hearing loss, tinnitus, fullness, otolgia, aural discharge. Previous otologic surgery or trauma
- Balance: Description of first episode of vertigo/dizziness/imbalance
- Number and frequency of attacks
- Length of attacks
- Exacerbating factors: particular movements, dietary or other environmental factors
- Associated symptoms, especially neurologic
- Degree of impact on everyday life
- History or family history of migraine
- History of head trauma, external or barotrauma
- History of possible ototoxic medications
- Cardiovascular risk factors
- History of any other conditions affecting peripheral sensory inputs, such as diabetes mellitus, osteoarthritis, previous joint surgery.
The goal of a structured history and examination is to identify a vestibular from non-vestibular causes of vertigo, and peripheral from central.
A strong suspicion of the cause of vertigo is often deduced during a careful history. The site, degree of lesion, single or episodic, unilateral or bilateral, provocative events, associated symptoms and degree of compensation are the answers to extract from history.
Clues from associated symptoms: The site of lesion will determine possible associated symptoms
Inner ear: hearing loss, tinnitus, fullness and otalgia.
Internal auditory canal and CPA: hearing loss, tinnitus, facial weakness, facial numbness, incoordination.
Brainstem: diplopia, dysarthria, long tract signs, Horners syndrome.
History is followed by a thorough neuro-otologic examination
The Neuro-Otologic Examination
- Which is the better hearing ear ?
- Otoscopy: Pneumatic otoscopy and tragal pump
- Tuning fork tests: 512Hz
Weber [midline versus lateralisation]
Rinne [positive, or normal means air conduction is better than bone conduction]
- Screening tests of hearing
Whisper test [a whisper heard at arms length whilst masking the other ear by rubbing the tragus suggests thresholds below 30dB]
- The eyes; assess for spontaneous or gaze evoked nystagmus. Use frenzel glasses if available [removes visual fixation that can suppress nystagmus of a peripheral cause]
- Head impulse test
- Romberg and stress Romberg. Use a foam mat if available [or two pillows]
- Gait assessment
- Dix-Hallpike manoeuvre
- Cranial nerve examination
- Cerebellar and long tract examination, including tests of proprioception
Head impulse test
Rapid movement of the head testing the horizontal VOR. The patient is asked to fixate on the examiners nose. A short, rapid rotation of the patients head is made by the examiner. An abnormality of the peripheral vestibular system is evident if the eyes follow the head movement and then snap back to regain fixation on the examiners nose. In addition you can ask the patient to shake their head rapidly for 10 seconds, with their eyes closed. This can uncover the presence of nystagmus.
Romberg test
The aim of this test is to isolate various sensory inputs contributing to the ability to maintain a steady posture.
Initally test the patient standing unassisted with feet together. Consider a cerebellar or other central abnormality if significant instability already exists. If significant increase in instability occurs with eye closure consider a vestibular cause. Next place in heel toe position [this is referred to as the stress Romberg test] eyes open first then eyes closed. Ideally, repeating this test again with the patient standing on foam mat [or 2 pillows], with the eyes closed removes both visual and proprioceptive inputs, often uncovering a severe unilateral, or bilateral vestibular lesion.
Stepping test
The patient is asked to march on the spot, with high steps, eyes closed and arms outstretched. Try at least 30 steps. A peripheral vestibular lesion will often manifest as a rotation toward the side of the lesion.
Dix-Hallpike test
A test designed to diagnose BPPV of the posterior canal. The patient is initially in a sitting position. Next rapidly lower the patient on to their back so their head is hanging off the edge of the bed, and rotate initially to the right. This places the plane of the posterior semi-circular canal in the vertical with the ampulla uppermost. If otoconia are present, they will fall with gravity, dragging the endolymph away from the ampulla, and thus stimulating this canal. This is manifest as a sensation of rotatory vertigo, after a short latency, and is accompanied by a fast beating nystagmus in a geotropic direction. ie in a torsional direction toward the floor. Repeat this with the head turned to the other side.
Repositioning Manoeuvres
The goal is to move the otoconia present in the semi-circular canals back in to the vestibule, where they are unable to stimulate the crista ampullaris, thus causing the illusion of rotation.
Oucnce the Dix-Hallpike test has been performed and a positive result obtained, keep the patients head in that position until the sensation of rotation and nystagmus has abated. Then slowly turn the head through 180 degrees. Then the patient turns first on to their side and then onto their front, while at all times keeping their chin tucked in to their chest. Then assist the patient back to the sitting postion. Advise the patient to avoid provocative postions, avoid lying on the affected side, and to sleep on a couple of pillows for the next few days.
Further testing is usually required. Most patients will require referral for a pure tone audiogram.
Important points on audiology
- In the acute setting the presence of a sensorineural hearing loss usually suggests involvement of labyrinth
- A documented hearing loss is a prerequisite in the diagnosis of Meniere’s disease [Initially a low tone loss is seen]
- Normal in migraine and BPPV
- Asymmetrical sensorineural hearing loss. The presence of greater than 10dB difference in 2 more frequencies is a criteria for MRI scanning to exclude an acoustic neuroma [also known as a vestibular schwannoma]
Laboratory testing of vestibular function is also helpful, however extreme care must be taken to ensure useful information. A reputable laboratory such as the hearing and balance centre St Vincents hospital is essential.
Tests
Pure tone audiogram
Caloric testing
Imaging
CT scans of the petrous temporal bone
MRI scans of the brain,brainstem and internal auditory canals
Blood tests
Assessing for rare inflammatory causes of inner ear disorders
[CRP, auto-immune screen, FTA-ABS]
Understanding Nystagmus of a Peripheral Vestibular Lesion
Spontaneous nystagmus most commonly is the result of a peripheral vestibular lesion. It is the manifestation of an imbalance of inputs from the vestibular nuclei to the oculomotor neurons.
The vestibular nuclei in the brainstem discharge at a tonic rate, even at rest. For instance:. if a sudden lesion affects the right vestibular pathway, the tonic discharge of the left vestibule predominates, giving the sensation of rotation to the left. The vestibulo-ocular reflex [whose aim is to keep an object fixed on the retina], will guide the conjugate gaze to the right [in relation to the head]. This eye movement can only travel a certain distance, so the compensatory movement is a fast catch-up saccade to the left. By convention it is the fast correction that determines the annotation of the direction of nystagmus. In summary, in most cases involving an acute peripheral vestibular injury the fast phase of the nystagmus is away from the side of the lesion.
Bidirectional or vertical nystagmus suggests a central lesion. Additionally nystagmus caused by a peripheral lesion is suppressed by visual fixation.
Interestingly, in an acute peripheral lesion, looking toward the direction of the fast phase of nystagmus will increase the degree of nystagmus.
The first episode of vertigo:
This can be a devastating experience for the patient, especially if this is acute onset sustained vertigo.
The most important initial step is to differentiate a cerebellar or brainstem cerebrovascular accident from labyrinthitis or vestibular neuronitis: ie central from peripheral cause. The patients age and cardiovascular status is important, as is a history of previous episodes of vertigo or any symptoms related to the ear. The presence of an abnormal head impulse test, and the absence of truncal or limb ataxia and long tract signs makes the likelihood of a brainstem/cerebellar lesion very unlikely. If there is any concern an urgent referral to hospital for an MRI and neurological assessment is mandatory.
The most likely diagnosis includes vestibular neuronitis, acute labyrinthitis. These lesions are often described as acute unilateral vestibulopathy.
Vestibular neuronitis is often heralded by severe vertigo and vomiting, building over a 24 hour period. Importantly while the patient is unsteady, they should be able to stand unaided. A viral or microvascular insult is thought to be the underlying cause. A short course of vestibular suppressants is reasonable [Benzodiazepines are the most effective at controlling vertigo, with prochloperazine helping control nausea]. Early weaning and mobilisation is essential to encourage compensation of the contralateral vestibule. It is also prudent to arrange an MRI of the brain and brainstem to exclude other pathology that can albeit rarely, present in this fashion.
Acute labyrinthitis is the result of inflammation of the membranous labyrinth, thus affecting both vestibular and cochlear function. Usually an obvious cause is not found, however suppurative middle ear or mastoid disease can secondarily affect the labyrinth.
Other considerations must include trauma, either closed head injury or barotrauma, a situation suggested on history. In addition this could represent the first episode of BPPV, migrainous vertigo or a complication of chronic otitis. Vertigo caused by otherwise uncomplicated acute otitis media is very rare, and other causes should first be excluded. Also rarely other non-infectious inflammatory causes can result in this condition This includes auto-immune disorders and syphilitic otitis.
The severity and length of symptoms relates to the degree of the lesion, the speed at which the lesion occurs, and the functional status of the opposite vestibular system. The severe vertigo caused by an acute vestibular insult rarely extends longer than a week. A young otherwise healthy person will usually make a full recovery. The more elderly population often take longer to compensate, and can often be left with a mild to moderate dysequilibrium.
Hallmarks of a peripheral vestibular lesion
- Often associated with significant autonomic symptoms: pallor, sweating, nausea and vomiting
- Exacerbation with head movement
- Positive head impulse test: a refixation saccade noted on rapid head movement toward the side of the lesion
- Instability, but the ability to stand unaided
- The absence of limb or truncal ataxia which suggests a cerebellar lesion
- The absence of long tract signs or other cranial nerve lesions APART FROM A CHANGE IN HEARING
- Nystagmus; uni-directional horizontal with torsional component
Causes of Episodic Vertigo
This is a far more common diagnostic dilemma.
The classic text book division of episodic vertigo does retain some utility.
Seconds-minutes =BPPV
Minutes –hours =Menieres disease
Hours-days=Migraine
Benign positional paroxysmal vertigo
The commonest cause of vertigo is BPPV. This is a condition caused by mobile particles within the semicircular canals, producing increased drag and stimulating the vestibular hair cells. This most commonly occurs in the posterior canal supplied by the inferior division of the vestubular nerve. Classically it is triggered by head movements with a few seconds latency; looking up or rolling over in bed, causing an intense rotatory sensation usually lasting less than 30 seconds. This can often be followed by the feeling of instability. Patients often describe their attacks occurring in clusters, a number of times a day for a few weeks at a time. Obviously, depending on the situation where this occurs this can be a severely debilitating condition. There are also legal implications especially for those holding a heavy vehicle liscence. [Check out the RTA website to obtain a copy of these guidelines]. Whilst these attacks will often subside spontaneously, repositioning manoeuvres are very successful in curing this condition. Unfortunately you need to see the patient during an active phase of their illness, and as in much of the investigation of vertigo it is important to allow patients to see you at short notice during an active phase of symptoms.
Migraine
This a highly prevalent disease in the community, and should be strongly considered as a cause of episodic vertigo, head motion intolerance and dysequilibium, especially in the younger otherwise healthy population. It is thought that 20-40% of those with migraines will suffer episodes of true vertigo. These may or may not be temporally related to their headaches. Importantly migraine is almost never associated with a hearing loss, and the patient will have normal caloric testing.
Menieres disease
MD has been a fascination to the otologic and wider medical community for a long time. It is a disorder that is related to a imbalance in the internal homeostais of the inner ear, manifesting itself in the form of episodic vertigo, documented fluctuating hearing loss, tinnitus and aural fullness. Attacks of vertigo usually last a couple of hours, followed by a period of dysequilibrium. Attacks can last much longer, and the frequency can be such as to be significantly debilitating. The natural history is one of progressive sensorineural hearing loss, with vertigo spells eventually tending to burn out. The incidence of bilateral disease is thought to be approximately 20% over a 20 year period. Stepwise management involves firstly dietary salt restriction, then a trial of diuretics, meausures which will control approximately 80-90% of patients. For those with more severe disease consideration of gentamicin application to the middle ear, endolymphatic sac surgery or vestibular nerve section is made.
Chronic Otitis
The presence of chronic inflammation of the middle ear can lead to bony erosion of both the ossicles, leading to a conductive hearing loss, as well as the otic capsule resulting in both sensorineural hearing loss and vestibular dysfunction. The most aggressive form of this disease occurs with the presence of cholesteatoma. This is defined as the presence of keratinising stratified squamous epithelium within the middle ear cleft, that has the ability to migrate and to erode bone. Apart from the ossicles, it is the lateral semicircular canal that is most commonly eroded. This condition is somewhat erroneously called a lateral canal fistula. This results in a communication between the middle ear and the membranous labyrinth. Therefore pressure changes, or even changes in the temperature of the air or fluid in the area can stimulate the vestibule giving the sensation of movement. This situation can also be apparent after performing a modified radical mastoidectomy. Therefore it is important when examining a patient with chronic ear disease to conduct a fistula test. This is done by applying pressure through a pneumatic bulb attached to the otoscope [a seal with the ear canal must be made]. If this is not possible, application of pressure over the tragus can also be used. A positive test is suggested when the vertigo is elicited and or the presence of eye deviation is noted.
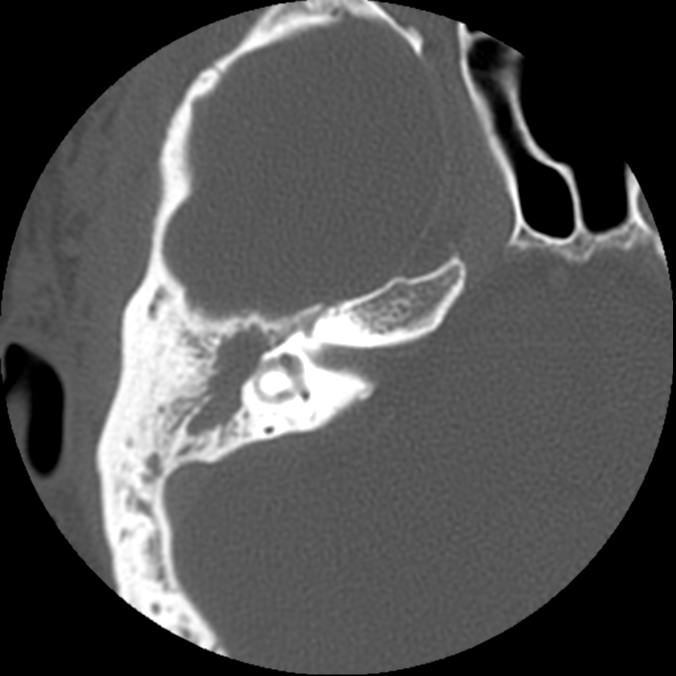
Lateral semicircular canal fistula. Axial CT scan showing widespread opacification of the middle ear cleft, with erosion of bone over the lateral semicircular canal
Another cause of a so called 3rd window into the vestibule is the recently described condition called superior canal dehiscence syndrome. (See seperate entry) This is a rare entity where a patient describes pressure and noise induced vertigo, due to a loss of bony coverage of the superior canal in the middle cranial fossa. A fine cut CT scan of the temporal bones, ideally orientated at right angles to the superior canal, with a battery of vestibular function tests can help identify this condition.
Trauma
Closed head injuries can result in significant morbidity. If this injury involves the temporal bone, the patient can suffer from permanent complete sensorineural hearing loss, and facial nerve injuries in addition to vestibular loss. Fortunately, if the contralteral vestibular function remains intact, almost complete compensation is made of several weeks to months. As with all vestibular injuries, limiting the degree of vestibular suppression [through medications] and increasing the level of mobility will speed this compensatory process.
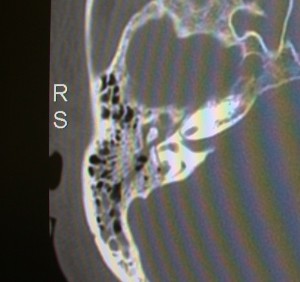
Coronal CT scan of the temporal bones. The mastoid air cells are filled with blood. A fracture line is seen travelling through the otic capsule which has resulted in a complete vestibular and hearing loss on this side.
Whilst uncommon barotrauma can also cause injury to the labyrinth. Scuba diving is the activity that can potentially expose the middle and inner ears to the largest pressure changes. The mechanism is either a rupture and leak of perilymphatic fluid, or the development of inner ear decompression illness. A situation such as this necessitates rapid specialist referral.
Other neurological conditions
Transient ischaemic attacks: by definition a transient neurologic dysfunction almost always associated with other neurologic signs and symptoms.
Multiple sclerosis rarely presents with vertigo, but dizziness or dysequilibrium are not uncommon during the course of the disease.
Dysequilibrium
Imbalance arising from abnormalities of the peripheral vestibular system are usually the result of a slowly progressive unilateral lesions, or the bilateral loss of vestibular function. Dysequilibrium that is present at all times, and exacerbated by head movement is suggestive of a vestibular problem. This is in contrast to a person who is unsteady or dizzy when walking, but is comfortable sitting in or driving a car, where assessment of other neurologic systems is warranted.
A history or evidence of chronic ear disease necessitates a careful otologic assessement. The presence of asymmetrical hearing or tinnitus raises the possibility of an abnormality in the cerebello-pontine angle, most commonly a schwannoma of the vestibular nerve [more commonly called an acoustic neuroma].
Bilateral vestibular loss can be difficult to prove. A history of gentamicin or other ototoxics given, or prior head trauma should be taken. The Romberg test conducted whilst the patient is standing on a thick sponge can uncover significant instability. Bilateral abnormalities of the head impulse test, as well as oscillopsia [a sensation of the world bobbing up and down whilst walking] can also suggest a bilateral peripheral vestibular lesion, prior to caloric testing.
Recovery and Rehabilitation
As mentioned above the balance system is comprised of many inputs. Following an injury to one of these inputs the brain attempts to compensate for the imbalance created. From a vestibular perspective loss or partial loss of one vestibule can take weeks to months. In a young and otherwise healthy patient this recovery is usually near complete, with residual problems noted only noted on rapid head movement and in extreme conditions. Following an acute injury minimisation of vestibular suppressants is important, as is early mobilisation and VOR (vestibulo-ocular reflex) exercises. Most people can do these themselves but in the elderly population consultation with a physiotherapist trained in vestibular rehabilitation is very important.
In some cases, however, this compensation does not occur, often due to multifactorial deficits, the lack of brain plasticity (declines with age), and anxiety can be a driving factor in limiting compensation. This situation is often labelle d psychophysiologic dizziness. In these cases not only physical vestibular rehabilitation is important but so too is pyschological retraining.
In Summary
Dizziness and vertigo are common problems, with peripheral vestibular disorders responsible in a significant percentage. Whilst the assessment and management of these disorders often requires multi-disciplinary involvement, a targeted initial approach will uncover the underlying cause in many cases.
Keeping the possibility of an acute cerebrovascular event in mind in the work-up of acute vertigo is important.
Chronic symptoms are rarely due to life threatening causes but often impact significantly on every day living.
