Otitis Externa
In general terms otitis externa (commonly called swimmers ear) is an inflammation of the skin of the auditory canal. This is usually a primary infection, but can occur as the result of discharge from the middle ear. Distinguishing this, especially in children can be difficult.
In order to understand otitis externa, understanding the anatomy and physiology of the external auditory canal is important.
The external auditory canal is comprised of cartilaginous and bony segments. The skin covering the external cartilaginous component is thick, hair bearing and produces cerumen (wax), with cerumen acting as both a waterproofing as well as an antibacterial and antifungal agent.
The skin covering the bony component is not hair bearing, is unique in that there is no subcutaneous tissue separating it from the bone, and that in most people the skin migrates from medial to lateral, extruding itself from the canal: ie it is self cleaning. Any factor that interferes with the normal functioning of the external auditory canal can predispose to infection.
Classic features of otitis externa
- Significant pain with tenderness on manipulation of the pinna
- Swelling of the canal and hearing loss
- Non-mucoid discharge
- Usually an history of water exposure and/or trauma to the skin of the ear canal.
Predisposing factors
Narrowing of the canal. There is a wide variation in the diameter of the external auditory canal. Severe congenital narrowing is rare as are exostoses in the paediatric setting.
Dermatitis of the skin of the canal is surprisingly common.
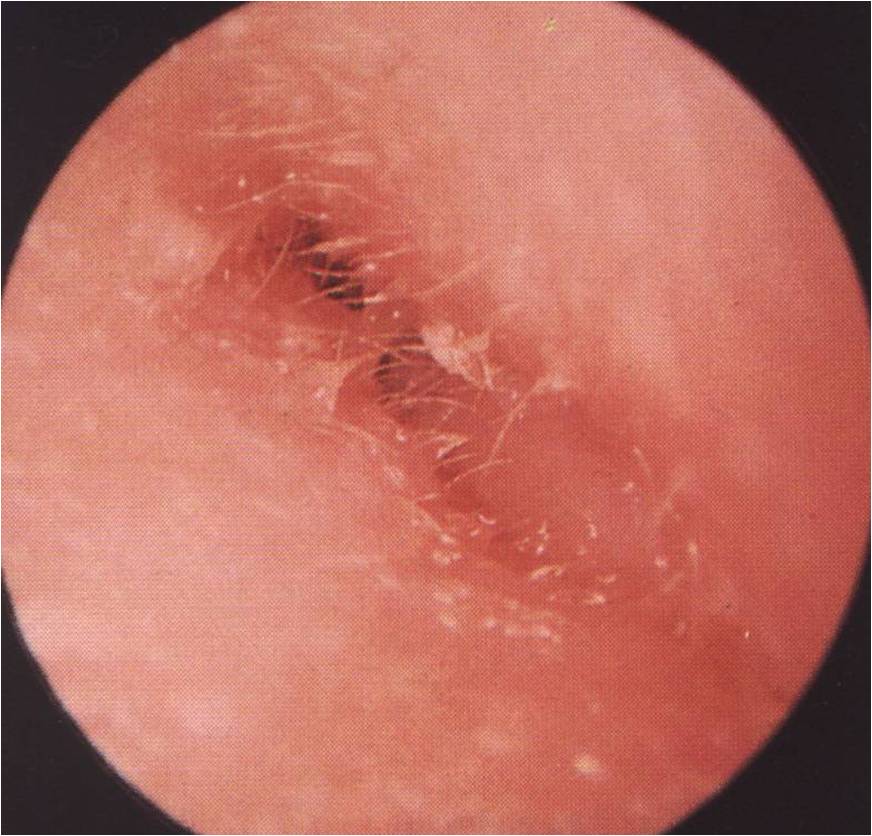 Note the severe swelling causing occlusion of the external auditory canal, with only a minimal degree of discharge seen.
Note the severe swelling causing occlusion of the external auditory canal, with only a minimal degree of discharge seen.
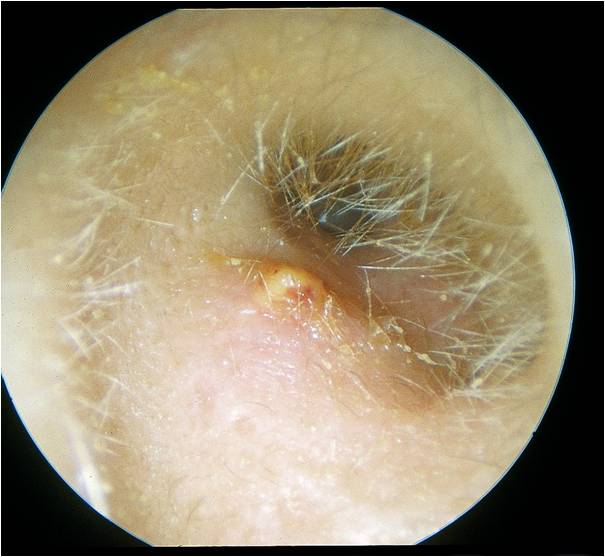 Note the localised abscess formation. Whilst most OE is generalised less commonly a furuncle can form in association with a hair follicle.
Note the localised abscess formation. Whilst most OE is generalised less commonly a furuncle can form in association with a hair follicle.
Commonest organisms:
Pseudomonas aueroginosa
Staphylococcus aureus
Gram negative rods such as Klebsiella and E.Coli
Fungi are responsible for approximately 10% of cases with Aspergillus species the most prominent.
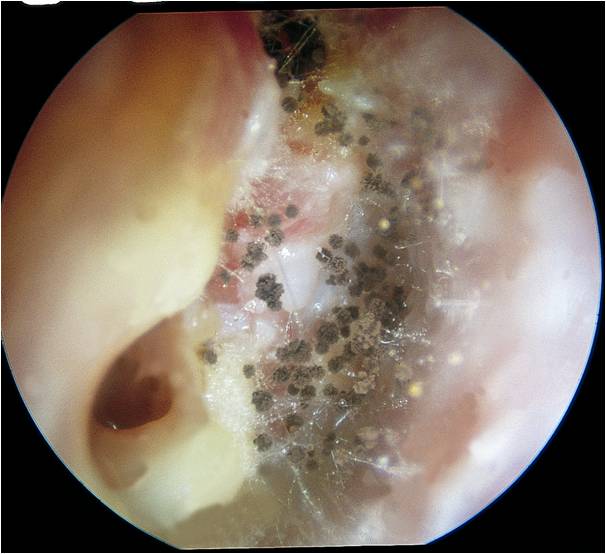 Aspergillus niger otitis externa
Aspergillus niger otitis externa
Post treatment fungal colonisation and chronic fungal otitis externa are not uncommon entities.
Management Essentials
Correct diagnosis: especially in children there is a often a difficulty in determining whether a presentation of otalgia is the result of otitis externa or of the more common acute otitis media, especially if this is associated with a tympanic membrane perforation. (Discharge from the middle ear usually has a mucoid nature.)
Ear toilet: the commonest cause of treatment failure is inability to apply topical therapy. Without access to a suction device and a microscope, the use of a cotton wool ball fashioned into a spear can allow removal of a degree of discharge from the ear canal. Severe swelling of the skin and extreme tenderness also limits adequate toilet. Ideally therefore microscopic toilet with a suction aspirator is required, and this may be needed every couple of days.
Topical therapy: most otitis externa is treated successfully with topical therapy. The important components of this therapy are the acidity and anti-inflammatory components as well their the anti-microbial activity. If you are confident that the tympanic membrane is intact, sofradex is the first line therapy. A ciprofloxacin based drop should be used when a tympanic membrane perforation is a possibility.
When a fungal infection is suspected, ear toilet is even more important. Topical therapy available includes kenacomb and locacorten-vioform drops.
Water exclusion is vital
A very important part of management is analgesia. The use of topical steroids and resolution of the infection are critical but systemic use of NSAIDs and paractemol is also important. In very severe cases adding a short course of prednisone can assist.
Complicated Cases
Microbiological diagnosis for recalcitrant cases
Severe swelling of the canal: Oral antibiotics and a short course oral steroids can allow initial resolution of swelling then allowing topical therapy to be more effective. The fact that pseudomonas represents the commonest bacterial cause of OE does represent problems in selecting an appropriate agent, given that oral ciprofloxacin is problematic in the paediatric setting.
Referral for microscopic toilet: this allows effective removal of debris and purulent discharge. It also allows exclusion of the presence of a foreign body (always a consideration in children).
Insertion of a wick: a self expanding wick inserted into a narrowed canal allows delivery of topical therapy with continuous exposure to the antimicrobial agent. This is usually removed at 48-72 hours.Another option for difficult cases is the instillation of anti-microbial, anti-fungal and anti-inflammatory ointments to fill the canal under direct microscopic guidance.
Oral antibiotics for systemic symptoms, spreading cellulitis or middle ear involvement.
Complications of otitis externa
Whilst rare the following can develop:
Cellulitis: spreading cellulitis involving the pinna, face and upper neck. More seriously is the development of perichondritis
Secondary acute otitis media
Tympanic membrane perforation
Malignant otitis externa (skull base osteomyelitis): essentially isolated to the immunocompromised.
Complete stenosis of the ear canal following recurrent infection.
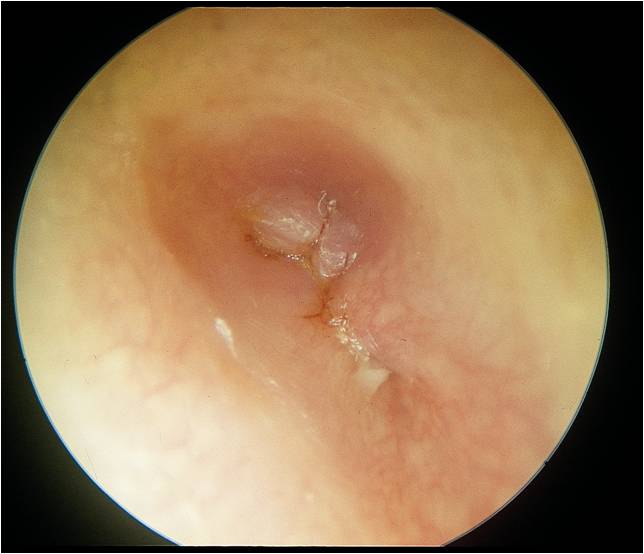 Note complete occlusion of the canal leading to significant hearing loss.
Note complete occlusion of the canal leading to significant hearing loss.
Long term avoidance
Water precautions: for those prone to recurrent infections the use of cotton wool with Vaseline in the bath and shower, and fitted ear plugs for swimming. When retained water is suspected, the intermittent use of a alcohol based drop such as Swimmers ear drops is useful.
Avoid skin trauma: no cotton buds or scratching
Simple intermittent use of olive oil drops can be very useful for minimising wax buildup, dryness and itching.
Identification and treatment of underlying dermatitides. Atopic dermatitis, contact dermatitis (including that to components of topical therapy) , psoriasis amongst others should always be considered. Topical steroids are often indicated and the use of hypoallergenic skin and hair products recommended.
Management of underlying middle ear disease with perforation.
