Natural history of growth is critically important in the formulation of a management paradigm.
A renowned pathologist Schuckneckt estimated an incidence of 0.57% on review of 1400 temporal bones. The National Institutes of Health Consensus Statement estimated an incidence of around 1 per 100,000 per year. The inference is that a significant number of tumours never become clinically apparent.
Treatment algorithms include conservative surveillance, microsurgical removal employing either hearing conservation or hearing destructive approaches and radiotherapy. There have been increased reports on quality of life outcomes, as well as large series reporting complications, hearing and facial nerve conservation rates.
The critical decision to be made is when to intervene. One of the most important questions to answer revolves around 1) what aspect of the tumours existence most disables the patient and 2) does early intervention realistically improve or arrest the progression of this disability without introducing the morbidity of the treatment itself. The two most easily quantifiable variables are hearing scored via PTA (pure tone average) and SD (speech discrimination), and facial nerve outcomes HB I-VI (with grade I meaning normal facial movement, to grade VI meaning complete paralysis). Clinical and laboratory evaluation and optimisation of balance are also critical. The increased use of QOL (quality of life questionaires) , both specific, such as hearing disability scores, and generalised such as SF-36, are broadening the information for analysis, and hopefully allowing us to make more informed decisions and recommendations for appropriate management.
The St Vincent’s Otology and Skull Base Unit has been conducting a prospective study on the management of vestibular schwannomas for over 10 years. In addition to collecting data related to the tumour size and growth patterns, hearing and balance, and facial nerve function, we ask those patients enrolled in the study to fill out quality of life surveys each year, with aim of better assessing their overall level of functioning and changes over time. We would welcome any patient diagnosed to enrol in this study which involves regular clinical and radiologic review and assessment of quality of life parameters.
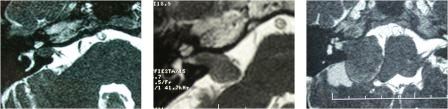
These figures show the varying sizes of tumours that are identified. The first image shows a small black mass within the internal auditory canal, through which the nerves of hearing and balance and the facial nerve travel from the brain into the ear itself. The second image shows that a tumour has extended outside this canal and is now occupying the cerebellopontine angle (CPA), coming close to the brainstem. The third image shows a tumour that has grown to the degree where there is compression of the brainstem.
As a general principal many small tumours as in the first image are initially monitored and intervention is made when and if growth can be documented, or if in specific circumstances a decision is made to attempt to preserve residual hearing. The size seen in the second image needs close observation, and consideration of early intervention. Certainly tumours at the size seen in the third image require interventional management soon after diagnosis.
Conservative Management
A reasonable option for management for most small to medium sized tumours. This is related to the natural history of many of these tumours being that they do not grow following diagnosis. If appropriate, an MRI scan is first repeated after 6 months to determine if there has been any growth. If the tumour and symptoms remain stable scans are then repeated yearly for at least 5 years.
Whilst there is no active intervention for the tumour itself, balance retraining and options for hearing rehabilitation are strongly pursued. It is also important to ensure that the patient has the appropriate clinical and social supports.
The ‘failure rate’ of conservative therapy is now 15-20%, which means that interventional treatment is required after an initial period of observation.
Many studies have explored relative QOL outcomes: the summary of these studies is that even for those tumours who fail initial conservative treatment, quality of life outcomes are not worse than if treated at initial presentation.
Certainly there remains a strong role for surgery in the management of vestibular schwannomas (acoustic neuromas), but just because a tumour is there does not mean that it must be removed.
When to proceed to surgery
- Documented growth: Usually greater than 2-4mm per year. Intervening when the tumour is less than 15mm in the CPA gives the best results.
- Brainstem compression
- Significant vestibular disturbance: occasionally even for small tumours
- Selected cases in small tumours where hearing preservation is considered
Surgery
The principles are to widely remove bone at the base of the skull in order to identify and protect neural structures. The surgery itself is highly technical and requires a dual surgeon approach. Dr Flanagan and his colleagues at the St Vincent’s Skull Base Surgery department perform the highest volume of acoustic neuroma surgery in Australia, with all surgeons dual fellowship trained. One of the most challenging aspects of surgery, especially in larger tumours is preservation of the facial nerve while optimising complete removal of the tumour.
The commonest route is trans-labyrinthine, followed by the retrosigmoid and the middle cranial fossa approach.
Radiotherapy
Steriotactic radiotherapy is an option for small to medium sized tumours with documented growth, in patients in whom surgery is contra-indicated, and in cases where residual tumour shows regrowth. I would encourage a review and opinion from one of our radiotherapy colleagues.
Summary of Management of Vestibular Schwannomas (Acoustic Neuromas)
The management decisions and the complexity of surgery make the importance of choosing a unit with a vast experience in the treatment of these tumours essential. Please contact us if you would like further information.
The department has been running a prospective research study for over 10 years. This involves monitoring consented patients who have been diagnosed with a vestibular schwannoma. Details regarding the tumour size and growth, hearing and balance, and overall quality of life are analysed.
Please click on this link for further information. Management of Vestibular Schwannomas and other Skull Base Tumours.
